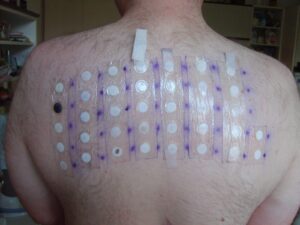
Patch Testing By Jan Polák
Just over a year ago, an allergist gave me a patch test that changed my life. Those chemical-filled patches taped all over my back helped him to identify five contact allergens that answered a lot of questions about why I had been feeling so awful, inside and out. A year later I am still learning more and still trying to better understand my allergies. A year ago I asked my allergist whether I should avoid eating my contact allergens. His response was, “I don’t know. There’s no way I can test for that.” I have finally answered that question.
One of my strongest allergens from the patch testing was propylene glycol. I changed my medicated eczema creams, stopped using cough syrups, and made sure that every personal care and cleaning product in my house was propylene glycol free. I didn’t change my eating habits. I then learned that polyethylene glycol is a cross-reactor for propylene glycol, as a started to react to the polyester and spandex/lycra/elastane in my clothing (which are made using polyethylene glycol). Polyethylene glycol is a very similar (though not identical) molecule, and in some people the body is unable to differentiate between the two. This confusion means that the body reacts to both molecules as if they were the same. Over Christmas, I made a stop at a famous candy store from university and my diet changed a bit as we travelled. I ate more processed and junk foods than usual.
 Two and a half weeks ago, though, a new problem began. The right-hand side of my neck started to get tight. I don’t mean that I couldn’t move my neck, but there was obvious pressure under my jaw and all the way down to my collar bone, causing me to not be able to properly discern if my head was aligned properly while sitting or standing. Over days, that feeling grew into a tightening all the way around my throat. It wasn’t preventing breathing or swallowing, but it was very uncomfortable. In time, over a number of days, I started to identify a pattern. It wasn’t until just under two weeks in that I understood. The feeling would worsen within about 1/2 hour of eating certain foods, and then slowly lessen over the following several days. It was then that I contacted a friend with anaphylactic allergies and asked her if this sounded like a precursor to an anaphylactic allergy. She answered with a firm “Yes.”
Two and a half weeks ago, though, a new problem began. The right-hand side of my neck started to get tight. I don’t mean that I couldn’t move my neck, but there was obvious pressure under my jaw and all the way down to my collar bone, causing me to not be able to properly discern if my head was aligned properly while sitting or standing. Over days, that feeling grew into a tightening all the way around my throat. It wasn’t preventing breathing or swallowing, but it was very uncomfortable. In time, over a number of days, I started to identify a pattern. It wasn’t until just under two weeks in that I understood. The feeling would worsen within about 1/2 hour of eating certain foods, and then slowly lessen over the following several days. It was then that I contacted a friend with anaphylactic allergies and asked her if this sounded like a precursor to an anaphylactic allergy. She answered with a firm “Yes.”
What did I identify as a culprit? Propylene glycol. The same chemical to which I had tested strongly allergic in my patch test. You see, propylene glycol is used as a base (delivery system) for natural and artificial flavours and colours. Thus it was highly present in that candy and processed food I was eating. Propylene glycol is also used as a base in natural and artificial fragrances, but I had already been avoiding fragrances in personal care products because fragrances were identified as one of my allergens. Fragrances aren’t generally found in food, so there was no reason I needed to worry about them there. The other main chemical used for this purpose, glycerin, can be of either the vegetable glycerin variety or the chemically-formed glycerin variety. The chemically-formed glycerin is also identified by some propylene glycol allergy sufferers as a cross-reactor. Seldom does a manufacturer identify the base in the flavours, colours, and fragrances they use in their products, so this means that I need to avoid all natural and artificial fragrances, colours, and flavours.
 Anaphylactic allergies can escalate quickly and unpredictably. A tight throat one day can lead to full airway obstruction the next. Worried but nervous about the idea of having a life-threatening allergy, I went to my doctor. I told him about what I had been experiencing, and he prescribed Epi Pens, as I had expected. He said that it was unusual for an allergy to worsen into new symptoms like this, although it is not unusual at all for symptoms to worsen with continued exposure to an allergen. I told him about some of the other allergy symptoms I also experience, and he decided to send me for a blood test just to make sure that this is the only problem. My food intolerances to egg and dairy now pale in comparison to my propylene glycol allergy. I’ve become one of the Epi Pen carrying, food-allergic crowd. I can’t take chances, need to be over-cautious with everything I eat, and there is a good chance I won’t be eating at fast food restaurants ever again. All because my allergist didn’t know whether eating my allergens would be okay and I didn’t take the most cautious path forward.
Anaphylactic allergies can escalate quickly and unpredictably. A tight throat one day can lead to full airway obstruction the next. Worried but nervous about the idea of having a life-threatening allergy, I went to my doctor. I told him about what I had been experiencing, and he prescribed Epi Pens, as I had expected. He said that it was unusual for an allergy to worsen into new symptoms like this, although it is not unusual at all for symptoms to worsen with continued exposure to an allergen. I told him about some of the other allergy symptoms I also experience, and he decided to send me for a blood test just to make sure that this is the only problem. My food intolerances to egg and dairy now pale in comparison to my propylene glycol allergy. I’ve become one of the Epi Pen carrying, food-allergic crowd. I can’t take chances, need to be over-cautious with everything I eat, and there is a good chance I won’t be eating at fast food restaurants ever again. All because my allergist didn’t know whether eating my allergens would be okay and I didn’t take the most cautious path forward.
Not only can you experience an anaphylactic allergy, but you can experience longer-term allergy symptoms such as stomach upset or rashes hours or days after exposure to an allergen that causes anaphylaxis. That part has not been fun either, but it did help me to identify the cause of my anaphylactic reaction. The foods that seemed to cause stomach upset also appeared to be the culprits in the anaphylaxis reaction, and the itchy skin followed the first two reactions a day or two later.
 Two good things have come of this for me. First, I now have the power to end the symptoms I was experiencing and prevent them from happening again. Second, my body is pushing me more and more towards eating real foods without chemical additives. That can only be positive for me and my family. For the rest of you, I can unequivocally answer the big question: Yes, contact allergies can turn into food allergies, and continuing to eat foods that contain those contact allergens can lead to much worse outcomes.
Two good things have come of this for me. First, I now have the power to end the symptoms I was experiencing and prevent them from happening again. Second, my body is pushing me more and more towards eating real foods without chemical additives. That can only be positive for me and my family. For the rest of you, I can unequivocally answer the big question: Yes, contact allergies can turn into food allergies, and continuing to eat foods that contain those contact allergens can lead to much worse outcomes.
Have you had a contact allergen turn into a food allergen, or vice versa? What was the allergen, and what happened? Comment below.
